Author: John Ford, AIA, NCARB, EDAC, LEED AP | Senior Design Architect and Associate
How can hospitals be more resilient, flexible, and efficient in unprecedented and unpredictable situations? How can they improve the patient experience, outcomes, and staff efficiency and satisfaction?
In March 2020, as the COVID-19 pandemic began, our client – a Wisconsin-based healthcare provider – faced a significant challenge. They had only 34 beds available at one of their hospitals and projected demand of up to 250 beds by early May. Instead of setting up alternative care facilities that could disrupt staff workflow and safety, our client chose to modify its existing inpatient rooms, creating more intensive and intermediate care capacities. This innovative approach allowed them to respond dynamically to the pandemic’s changing needs. The effectiveness and efficiency of this solution left no doubt about the future direction of the inpatient infill project the provider had been considering: universal care rooms.
What are Universal Care Rooms?
Universal care rooms, or acuity adaptable rooms, represent a best practice in inpatient room design. Unlike traditional inpatient rooms designed for a specific level of care – such as ICU, intermediate care, or general care – universal rooms offer more flexibility. They can adapt to any level of care, allowing patients to stay in the same room throughout their hospitalization, regardless of changes in their condition or treatment needs. This adaptability inspires a new way of thinking about patient care, where the environment adjusts to the patient’s needs, not the other way around.
Starting in 2021, our team had the privilege of continuing an ongoing partnership with our client to implement 28 universal care rooms. The rooms have delivered high-quality care since they went live in 2023. What makes them successful are a few critical differences from traditional inpatient rooms:
- More infrastructure like additional medical gas outlets, electrical outlets and dialysis connection capabilities
- Increased clearances for emergency response, in-room procedures and life support equipment at the head of the bed
- A full bathroom with a shower
- Family space to promote family-centered care
- Windows for direct patient observation, which is required for ICU-level care
- An advanced patient vitals monitor, which can be controlled remotely from the hallway charting station
- Negative pressure capability, allowing treatment of patients with airborne infectious conditions like COVID-19, SARS or Tuberculosis
These features contribute to a more adaptable, efficient, patient-centered healthcare environment. They enable the hospital to swiftly adjust to varying patient needs without the logistical challenges of moving patients between specialized rooms. This flexibility is crucial in emergencies or when dealing with fluctuating patient acuity levels, ensuring the hospital can maintain the highest standard of care without delay. Moreover, including family space and direct observation capabilities supports not only the patient’s physical health but also their emotional well-being, making these rooms a holistic solution to patient care.
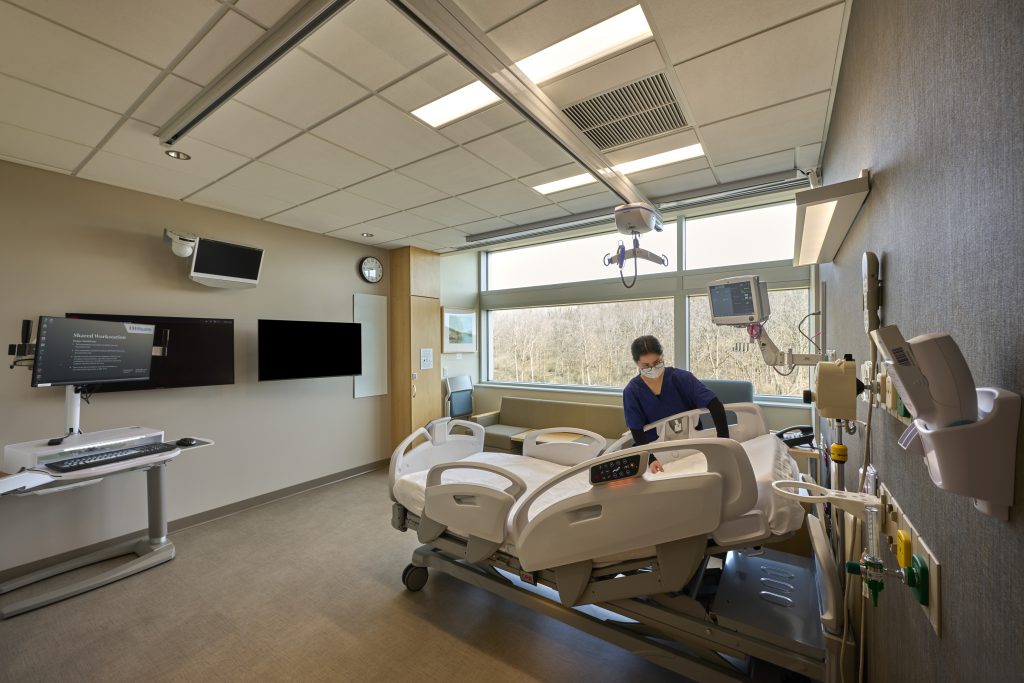
Universal care rooms are more adaptable than standard in-patient rooms and have the infrastructure required to treat a range of patient acuity levels.
A Win-Win for Patients and a Hospital’s Bottom Line
The flexibility of universal care rooms better equips healthcare providers to deal with mass casualty events, pandemics, or natural disasters, as they can quickly adjust the number and type of beds available to meet the demand. They also have specific patient and staffing benefits.
Universal care rooms improve the patient experience by eliminating the need for transfers between different units, which can cause stress and confusion, medical and medication errors, communication gaps, or patient dropping incidents. The rooms also reduce challenges associated with transferring patients with an airborne infectious condition – instead, patients can remain in the same room for their entire hospital stay. For patients requiring dialysis, in-room connections can enhance their experience by avoiding travel to another part of the facility. Reduced traveling also puts less strain and stress on visiting family members.
Universal care rooms integrate advanced technology to expand care access and overcome staffing challenges. Rooms usually incorporate telemetry, allowing for remote monitoring of patient vitals. Care teams can monitor patients via telemetry monitors placed in the nurse stations and along hallways. Many rooms also have electronic ICU (eICU) care equipment, bringing telehealth to the patient’s bedside. eICUs include a camera and a dedicated monitor, enabling specialists to conduct exams remotely.
Despite these benefits, many hospitals have – understandingly – been slow to adopt universal care rooms because of two primary challenges: up-front construction costs and qualified staff. However, both are easy to overcome if we consider the potential costs and challenges of not implementing universal care rooms.
When completing the universal care unit with our client, the team encountered higher initial costs from more medical gas, electricity, dialysis, eICU and equipment hook-ups, as well as the mechanical systems to accommodate positive and negative pressurization capabilities. However, these are small costs compared to the renovation and downtime in converting a typical inpatient unit to an ICU. Shutting down an inpatient bed wing for a 12- to 18-month renovation has a significant financial and operational impact. Universal care rooms allow hospitals to scale up their ICU rooms immediately without compromising the quality of care or the patient experience.
While design alone cannot solve staffing challenges, architects can help hospitals implement flexible spaces that empower health systems to provide the best possible care. These flexible spaces accommodate different patient acuity levels and the appropriate responses by the care team. They might include:
- Collaboration zones and nurses’ stations, which are the primary staff work areas and have sight lines to the universal care rooms
- Office-like workspaces, which are more private than the nurses’ stations and allow team members to work individually or collaborate on a patient’s treatment plan
- Focus rooms that are unassigned and available for various uses, such as a temporary charting area, a private area for small-group meetings or a quiet space for difficult conversations with family members
Equally important, these spaces may double as respite areas for staff to recharge and connect with their colleagues, which are essential for staff well-being and retention.

A staff-only area at our client’s universal care unit provides a place for connecting with colleagues, charting and respite space away from the patient’s bedside.
Design Considerations
Designing and operating universal care units is an exciting experience. Yes, there’s more to think about than when creating a traditional inpatient unit. Still, this part of the process offers opportunities to make the staff’s job easier and improve the patient’s experience. Here are a few design opportunities that require careful consideration and discussion between the design and stakeholder teams.
Visibility
Uninterrupted sightlines allow nurses to monitor patients better. Visibility becomes even more critical when the project team anticipates that the rooms will frequently treat high-acuity patients.
It is important to remember that universal care rooms are not meant to replace true ICUs, which always have high visibility into the rooms and typically have a nurses’ station across the hall for constant monitoring. Because they are designed to care for various patient acuity levels, universal care rooms may not always have this degree of visibility. Instead, they might have a centralized nurses’ station with decentralized charting stations outside the room. The design team should discuss with the hospital’s stakeholders the degree of visibility appropriate for each project.

Like ICUs, universal care rooms require clear sightlines from the corridors and nurses’ stations.
Toilet rooms
Full toilet rooms with a shower – instead of the dreaded Swivette or partitioned toilet often found in a traditional ICU – create a better patient and family experience. Generally, toilet rooms should be along the exterior wall or between every two patient rooms. Outboard or mid-board-nested-room designs provide maximum patient visibility from the corridor. They also make it easier for many team members and equipment carts to enter the room simultaneously, as is required when a patient codes or during other emergencies.
We opted for inboard toilet rooms at our client’s hospital because the infrastructure was already in place for this setup, which generated substantial cost savings. A project’s exact toilet room location will depend on the specific visibility requirements established by the care team and hospital leadership and the building’s existing conditions (if the project is a renovation).
Individuals of size
Universal care rooms can accommodate patients of different acuities, but individuals of size have different needs and challenges. They may also have higher risks of complications and need more staff assistance and monitoring. Patient lifts are typically incorporated in universal care rooms to transfer patients and reduce staff injury. Universal care units should include special rooms for individuals of size that have additional clearances for larger beds and toilet rooms. Special toilets, sinks, showers, and grab bars should be designed to accommodate these patients.
Positive-pressure rooms
Through the flexibility inherent to a universal care unit, pressurization can become negative in a bank of rooms, half the unit at one time, or through the entirety of the unit. These zones allow for better isolation and infection control of patients with airborne diseases. While negative-pressure rooms help prevent the spread of airborne diseases, positive-pressure rooms are needed for patients with weakened immune systems, such as those undergoing chemotherapy or organ transplants. Positive-pressure rooms create a higher pressure inside the room than outside. They prevent potentially contaminated air from entering the room, protecting patients from acquiring infections from the environment or other patients.
Space for staff and equipment
Universal care rooms have more staff space to accommodate intensivists, respiratory therapists, pharmacists, and other staff joining the care team as the unit flexes into high-acuity mode. Patients with higher acuity also have a greater demand for equipment, so the equipment storage rooms should have sufficient space for ventilators, dialysis, and other life support equipment.
Design Approach
Universal care rooms are a frontier for many healthcare providers. Perhaps more than any other hospital space typology, they require designers and engineers who know best practices, what works and the challenges a project team might face. These qualities come from experience and listening to and observing how hospital staff use the rooms and equipment. Our team used the strategies below at our client’s hospital to ensure a successful design.
Focus on the staff experience throughout the design process. We engaged staff because they are the primarily universal care room users. The input and feedback of the doctors, nurses, and support personnel running the rooms are invaluable in creating a functional and efficient design. We conducted surveys, interviews, workshops, and simulations with the staff to understand their needs, preferences and challenges. We incorporated their ideas and suggestions into the design.
Design with an integrated and Lean approach. These design approaches involve collaborating with the owner, contractor and consultants from the early stages of the project. We used Lean principles and tools to optimize the project’s value, quality, and efficiency, including Gemba walks, process mapping, and mockups to eliminate waste, reduce cost, improve safety and enhance performance. We also used 3D modeling and virtual reality to visualize and test the design and to communicate and coordinate with the entire project team and the staff.
Complete post-occupancy evaluations (POEs) to learn for the next project. Learning is continuous; every project is an opportunity to improve and innovate. After serving patients and staff for nearly a year, our client’s universal care rooms are undergoing a systematic assessment. We collect data and feedback from the staff, patients, and project team and analyze it to identify the design’s strengths and weaknesses and areas for improvement and enhancement. The results from these assessments will be available soon.
The lessons we learn from each project inform and guide the next one. For example, based on our experience, we helped our client move the charting stations—usually at the head of the patient’s bed—to the foot of the bed. This shift provides more space for other critical equipment to treat higher acuity patients.

The project’s design and construction team mocked up the headwall of a universal care room to help stakeholders test the room’s layout and equipment placements.
A Future-Ready Solution
Universal care rooms are vital to the future of healthcare, representing a move towards resilient and adaptable facilities. They also underscore the role of collaborative design in solving complex challenges, blending flexibility, technology, and a solid understanding of both patient and staff needs.
Implementing these rooms at our client’s hospital demonstrates their significant benefits: enhanced patient experiences, streamlined care delivery, and an improved capacity for the provider to manage emergencies and varying demands. This project sets a benchmark, showing the impactful role of architecture in health outcomes and operational efficiency.
Our team is prepared to offer insights and work alongside those looking to advance their healthcare facilities. This collaboration aims to address current challenges while preparing for what lies ahead. To learn more or to discuss potential projects, please reach out. Let’s work together to create better healthcare environments through strategic design and innovation.





 Alexandra Urrutia-Comas, MHSA, FACHE, is a distinguished healthcare leader serving as the Vice President of Operations at Aurora St. Luke’s Medical Center, a prominent healthcare institution within Aurora Health Care, now part of Advocate Aurora Health. With a Master of Health Services Administration from the University of Michigan and a Bachelor of Arts in Health Administration and Policy from the University of Maryland Baltimore County, Alexandra possesses a robust educational background complemented by over a decade of hands-on experience in healthcare administration. Her career journey includes progressively challenging roles, from her tenure as an Administrative Fellow at the Clement J. Zablocki VA Medical Center to her leadership positions at Wheaton Franciscan Healthcare and Aurora Health Care. Notably, Alexandra’s expertise extends to operations improvement, strategic planning, and executive leadership, underscored by her Lean Certified status and active engagement as a Wisconsin Regent for the American College of Healthcare Executives. Alexandra’s commitment to diversity, inclusion, and professional development is evident through her involvement in various organizations, including her current role as President of NALHE WI (National Association of Latino Healthcare Executives, Wisconsin Chapter). Her dedication to advancing healthcare leadership and fostering a culture of excellence makes her an invaluable asset to the healthcare community and beyond.
Alexandra Urrutia-Comas, MHSA, FACHE, is a distinguished healthcare leader serving as the Vice President of Operations at Aurora St. Luke’s Medical Center, a prominent healthcare institution within Aurora Health Care, now part of Advocate Aurora Health. With a Master of Health Services Administration from the University of Michigan and a Bachelor of Arts in Health Administration and Policy from the University of Maryland Baltimore County, Alexandra possesses a robust educational background complemented by over a decade of hands-on experience in healthcare administration. Her career journey includes progressively challenging roles, from her tenure as an Administrative Fellow at the Clement J. Zablocki VA Medical Center to her leadership positions at Wheaton Franciscan Healthcare and Aurora Health Care. Notably, Alexandra’s expertise extends to operations improvement, strategic planning, and executive leadership, underscored by her Lean Certified status and active engagement as a Wisconsin Regent for the American College of Healthcare Executives. Alexandra’s commitment to diversity, inclusion, and professional development is evident through her involvement in various organizations, including her current role as President of NALHE WI (National Association of Latino Healthcare Executives, Wisconsin Chapter). Her dedication to advancing healthcare leadership and fostering a culture of excellence makes her an invaluable asset to the healthcare community and beyond.
















